|
Most people recognise that heart attacks are a common cause of
death, particularly in the Western World. What is less well known
is that in many people with heart disease, the heart fails less
dramatically. The 'pump' function of the heart progressively
deteriorates, often gradually over a period of several years,
leading ultimately to 'pump' failure and, consequently, death –
this sequence of deterioration is called heart failure.
The combined figure for North America, Western Europe and Japan
for people affected by chronic heart failure exceeds 10 million.
In Europe, there are over 5 million patients with heart failure.
The number of patients developing heart failure per annum in the
UK is approximately 2.3 per 1000 members of the population and
over 400,000 new cases of heart failure occur every year in the
USA. Heart failure is extremely common and it is increasing world-wide.
What is Heart Failure?
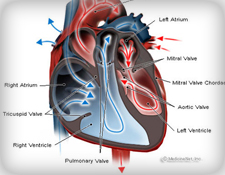
Heart failure is not a single disease but represents the endpoint
of a number of disease processes. The heart is normally a strong
muscular pump, able to drive blood throughout the body to maintain
the supply of oxygen. In heart failure, the pump function of the
heart gradually deteriorates, so that it is no longer able to meet
the body's metabolic requirements.
Congestive heart failure interferes with the kidney's normal
function of eliminating excess sodium and waste from the body. The
excess fluid retained causes swelling of the ankles and legs.
Fluid may also collect in the lungs – resulting in shortness of
breath. The severity of the condition and symptoms depends on how
much of the heart's pumping capacity has been lost.
The body can compensate for the deterioration in cardiac function
for some time, but in the long term it has a negative effect. At
first, the deterioration may only be noticeable by a shortness of
breath and fatigue when the individual puts stress on their heart
during exercise. Over time cardiac function deteriorates to the
point where the heart is no longer able to meet the body's
metabolic demands, even when the sufferer is at rest.
During the course of their disease, unless treated appropriately,
people with heart failure suffer a substantial loss of quality of
life and frequently have to be admitted to hospital.
Management of Heart Failure
The goal of treatment is to improve a person's quality of life by
making the appropriate lifestyle changes and implementing drug
therapy. Effective treatments exist to manage and improve heart
failure, including diuretics and ACE inhibitors. Most recently
drugs called beta blockers have been investigated for the
treatment of chronic heart failure and the evidence in favour of
beta blockade is strong. There are also diagnostic tests, for
early detection of heart failure and effective therapy monitoring.
Beta blockers - a major breakthrough in
heart failure management
When the body needs to increase the heart rate and the pump action
of the heart, such as during exercise, a hormone called
noradrenaline is released from nerves in the heart, and also from
the adrenal glands.
In a normal person, noradrenaline is released when it is needed,
such as during exercise. In patients with heart failure, huge
amounts of noradrenaline are released all the time to stimulate
cardiac function. This is the body's response to the heart not
working properly. By releasing lots of noradrenaline, the
sufferers' heart rate increases, but because the heart muscle is
damaged, this does not improve the function of the heart to a
great extent. In fact, it is now known that these high levels of
noradrenaline actually further damage the heart.
Understanding that these high levels of noradrenaline are bad for
the heart led to the idea that blocking the effects of
noradrenaline may be helpful in heart failure.
Beta blockers were then investigated for use in heart failure as
they block the beta adrenergic receptors in the heart through
which noradrenaline acts. For many years it was believed that beta
blockers would have a negative effect on heart failure patients
because it was felt that the increased noradrenaline levels were
useful in driving the failing heart. This was based on the idea
that if the pump was not working properly, increasing the rate of
pumping would help – in fact we now know that this is not the
case.
|