|
According to the World Health Organisation (WHO), osteoporosis is
second only to cardiovascular disease as a leading health care
problem. World-wide about one in three women and one in eight men
over the age of 50 risk having an osteoporotic fracture during
their lifetimes. Moreover, the number of hip fractures is expected
to increase from 1.7 million in 1990 to 6.3 million in 2050
because of the increasingly ageing world population.
Annual direct medical costs to treat an estimated 2.3 million
osteoporosis fractures in Europe and the United States together
amount to US$27 billion.
What is osteoporosis?
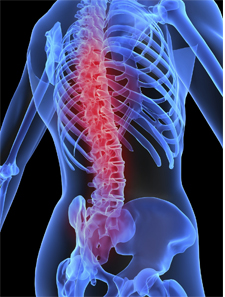
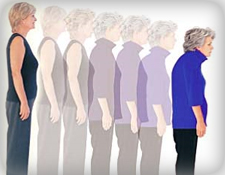
Osteoporosis is a disease affecting the bones which is
characterised by a decrease in bone mass and density that
increases the risk of broken bones, particularly in the spine,
wrist, hip, pelvis and upper arm. The disease occurs in women
after the menopause.
Unfortunately most people don't know they have osteoporosis until
they break a bone. As such, a new WHO study has stated that early
detection of low bone density could significantly reduce the
impact of osteoporosis.
Osteoporosis can be diagnosed relatively easily by:
medical history
basic investigations, including x-rays
bone mass density
– QCT (quantitative computed tomography)
– QUS (quantitative ultrasound scanning)
DXA (DEXA) dual energy x-ray absorptiometry
biochemical markers of bone turnover (serum + urine)
– bone formation
– bone breakdown
Management of osteoporosis
Strategies for the management of osteoporosis include:
A diet which maintains normal body weight throughout life and
provides a calcium intake of some 1000 mg per day from late
childhood onwards
Encouragement of a physically active lifestyle
Avoiding smoking and heavy drinking
Minimisation of cortisone use and potential administration of
osteoporosis prophylaxis medication when cortisone is given
Calcium and vitamin D supplementation
Drug therapy includes hormone replacement therapy in
postmenopausal women, bisphosphonates, and active vitamin D.
|